Digestive health in Singapore is the medical management of gastrointestinal (GI) and hepatic functions to ensure optimal nutrient absorption and systemic detoxification. In 2026, GI care will be integrated into the Healthier SG framework, prioritising early detection of conditions like colorectal cancer, fatty liver disease (NAFLD), and GERD. Specialist care in Singapore utilises advanced diagnostic protocols, including AI-augmented endoscopy and Fibroscans, to provide high-precision clinical outcomes.
What a Gastro Clinic Provides: Core Services and Definitions
A gastro clinic is a specialised medical facility dedicated to the diagnosis, treatment, and prevention of disorders within the alimentary canal and accessory organs. In Singapore, these clinics serve as the secondary tier of care for patients referred through the Primary Care Network (PCN).
Key clinical areas include:
- Upper GI Tract: Management of the oesophagus and stomach (e.g., gastritis, peptic ulcers).
- Lower GI Tract: Treatment of the small and large intestines (e.g., Irritable Bowel Syndrome, Diverticulitis).
- Accessory Organs: Specialised care for the pancreas and gallbladder (e.g., pancreatitis, gallstones).
Role of a Digestive & Liver Centre: Coordinated Care Models
A Digestive and Liver Centre is a multidisciplinary clinical hub that synchronises gastrointestinal medicine with hepatology (liver care) to manage complex metabolic and digestive disorders. This model is designed for “vertical integration”, where a single patient journey covers both diagnostic imaging and procedural intervention.
Benefits of Coordinated Care:
- Unified Diagnostics: Simultaneous evaluation of liver enzymes and gut microbiome health.
- Reduced Investigation Redundancy: Shared medical records under the National Electronic Health Record (NEHR) system prevent duplicate blood tests.
- Holistic Management: Treatment plans that address the “Gut-Liver Axis”, recognising how intestinal health directly impacts hepatic inflammation.
When Specialist Review Becomes Necessary: Identifying Red Flags
Clinical guidelines in 2026 mandate a specialist gastroenterology review if digestive symptoms persist for more than 14 days despite primary care intervention. Early referral is critical for the prevention of chronic disease progression.
Immediate Indications for Specialist Consultation:
- Dysphagia: Difficulty or pain when swallowing.
- Unexplained Weight Loss: A loss of >5% body weight within six months without lifestyle changes.
- Haematochezia: Presence of blood in the stool, requiring immediate Colonoscopy screening.
- Anaemia: Unexplained iron deficiency, which may indicate internal GI bleeding.
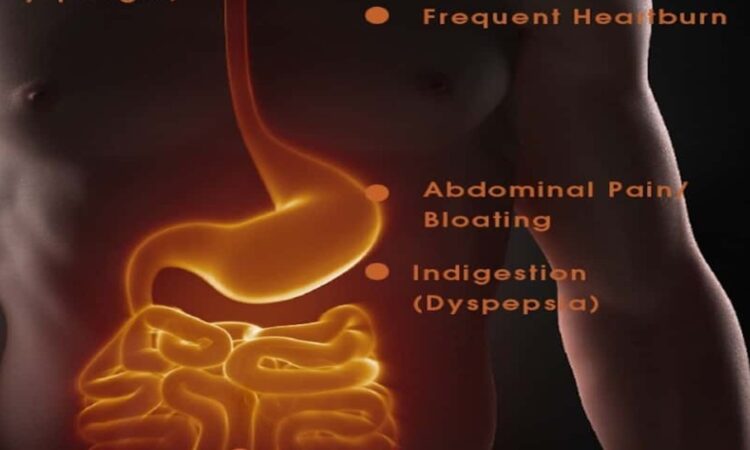
Common Digestive Symptoms Requiring Evaluation
Digestive symptoms are the physiological manifestations of underlying GI dysfunction, categorised by their location in the upper or lower tract. Understanding these symptoms is the first step in the Healthier SG care journey.
2026 Symptom-to-Specialist Reference Table
|
Symptom |
Potential Condition |
Recommended Initial Test |
|
Chronic Heartburn |
Gastro-oesophageal Reflux (GERD) |
Gastroscopy (OGD) |
|
Persistent Bloating |
Small Intestinal Bacterial Overgrowth (SIBO) |
Breath Test / Ultrasound |
|
Change in Bowel Habits |
Irritable Bowel Syndrome (IBS) |
Stool Calprotectin / Colonoscopy |
|
Upper Right Abdominal Pain |
Gallstones / Biliary Colic |
Hepatobiliary Ultrasound |
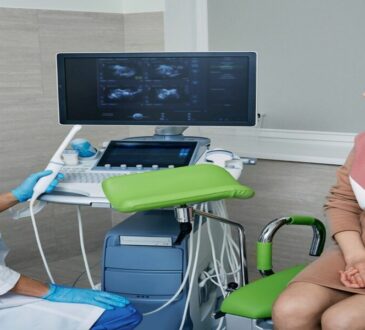
Diagnostic Methods in Gastrointestinal Care: The 2026 Tech Suite
Gastrointestinal diagnosis in 2026 utilises a “Triple-Assessment” model: clinical history, biochemical markers, and high-definition imaging. AI-assisted diagnostics have significantly reduced the “miss rate” for early-stage polyps and lesions.
- Endoscopy (Gastroscopy & Colonoscopy): Direct visualisation of the mucosa. In 2026, Computer-Aided Detection (CADe) highlights suspicious areas in real time.
- Non-Invasive Imaging: Specialised MRI (MRCP) for bile ducts and CT abdomen for structural reviews.
- Liver Stiffness Measurement: Utilising Fibroscan (Transient Elastography) to assess liver scarring (fibrosis) without a biopsy.
Managing Liver-Related Conditions (Hepatology)
Liver specialists (hepatologists) focus on the treatment of non-alcoholic fatty liver disease (NAFLD), viral hepatitis, and cirrhosis. With the rise of sedentary lifestyles, NAFLD has become the leading cause of liver dysfunction in Singapore as of 2026.
- Fatty Liver Management: Combines nutritional therapy with insulin-sensitising medications.
- Viral Hepatitis: Utilising high-efficacy antiviral therapies that can cure Hepatitis C in over 95% of cases.
- Detoxification Support: Monitoring the liver’s metabolic capacity via advanced blood panels (LFTs).
Treatment Planning and Follow-Up: The Longitudinal Approach
Treatment planning in 2026 is a collaborative “shared decision-making” process between the gastroenterologist and the patient.
- Medical Therapy: Use of biologics (e.g., for Crohn’s or ulcerative colitis) and acid suppressants.
- Lifestyle Interventions: Medically supervised diets (e.g., low-FODMAP) and stress-reduction protocols.
- Surgical Consultation: If conservative management fails, patients are transitioned to minimally invasive laparoscopic surgery.
Cost Planning and Affordability: Navigating Singapore’s Healthcare Schemes
Healthcare financing for digestive care in Singapore involves a combination of MediSave, MediShield Life, and Integrated Shield Plans (IP). Understanding these schemes is essential for cost-aware decision-making.
Financing Entities in 2026:
- MediSave 500/700: Can be used for outpatient chronic disease management, including IBS or chronic hepatitis.
- MediShield Life: Covers a large portion of inpatient surgical costs and selected outpatient treatments (e.g., colonoscopy for cancer screening).
- CHAS Subsidies: Blue and orange cardholders receive significantly subsidised rates at CHAS-accredited gastro clinics.
Preparing for Your Gastroenterology Consultation
Efficiency in clinical assessment is maximised when patients provide a “Digital Health Summary” through the National Electronic Health Record (NEHR).
- Medication Record: Include all supplements and Traditional Chinese Medicine (TCM), as these can impact liver enzymes.
- Family History: Specifically regarding colorectal or stomach cancers.
- Symptom Diary: Tracking “food-symptom” correlations for at least 7 days prior to the visit.
Long-Term Digestive Health Management
Sustainable digestive wellness in 2026 focuses on the “gut microbiome” and proactive screening.
- Annual Screenings: For individuals over 45, regular colonoscopies are the gold standard for cancer prevention.
- Nutrition: Emphasising fibre-rich diets and probiotic diversity to support intestinal immunity.
- Mental Wellbeing: Acknowledging the “Brain-Gut Axis”, where stress management directly reduces the severity of functional GI disorders like IBS.
Frequently Asked Questions (FAQ)
What conditions does a gastro clinic in Singapore manage?
Gastro clinics manage the full spectrum of digestive health, including GERD, stomach ulcers, Irritable Bowel Syndrome (IBS), Inflammatory Bowel Disease (IBD), and liver conditions like fatty liver.
When should I see a specialist for my bloating?
If bloating is accompanied by “red flag” symptoms like weight loss, blood in the stool, or severe pain, or if it persists for more than two weeks, a specialist review is clinically indicated.
How does a Digestive & Liver Centre improve patient outcomes?
By housing specialists in both GI and hepatology under one roof, these centres allow for a more comprehensive assessment of metabolic health, ensuring that liver issues are not overlooked in patients with digestive complaints.
Are diagnostic tests like colonoscopies claimable under MediSave?
Yes. In Singapore, colonoscopies performed for diagnostic purposes are claimable under the MOH Table of Surgical Procedures (TOSP) using your MediSave funds, within established limits.
Can lifestyle changes really fix liver issues?
For Non-Alcoholic Fatty Liver Disease (NAFLD), lifestyle changes, specifically weight loss of 7-10% and improved physical activity, are the primary treatment and can frequently reverse early-stage liver fat accumulation.
Taking Charge of Your Digestive Health in 2026
The landscape of digestive care in 2026 is moving toward value-based care and predictive diagnostics, prioritising prevention and gut-health optimisation over reactive treatment. For patients in Singapore, this means gaining access to tailored, proactive strategies that keep the digestive system functioning at its best. To explore personalised digestive and liver care solutions, schedule a consultation and take the first step toward a healthier gut.