Podiatric surgeons can treat foot and ankle pain that hasn’t improved with rest, ice, compression, elevation, or other conservative treatments. They treat foot, ankle, and leg conditions. They are also known as podiatrists and foot doctors.
When to see a podiatrist?
The following foot or ankle problems should be treated by a podiatrist:
- Chronic pain, swelling, redness, numbness/tingling in the feet or ankles that won’t go away
- Bunions or hammertoes that are causing significant pain or impacting your mobility
- Corns, calluses, or plantar warts that are very painful or interfere with walking
- Ingrown or fungal toenails that are recurring despite proper nail trimming and hygiene
- Limited range of motion, instability, clicking/popping sounds, or trouble bearing weight due to ankle sprains or other injuries
- Abnormal gait (walking pattern) resulting from structural foot problems or nerve issues
- Foot ulcers or wounds related to diabetes, poor circulation, or nerve damage that are slow to heal
- Bone spurs, arthritis, tendonitis, stress fractures, Achilles tendon injuries, or other chronic orthopedic conditions in the feet/ankles
If you have any symptoms like these that don’t get better within a couple of weeks with at-home treatment, make an appointment to see a podiatrist. The earlier you seek treatment for foot and ankle problems, the more options are available to help manage pain and prevent lasting damage.
What treatments do podiatrists provide?
Podiatrists have extensive medical training related to the foot and ankle. After earning a 4-year undergraduate degree, they complete a 4-year Doctor of Podiatric Medicine (DPM) program. Residencies and fellowships provide additional specialty training in areas like surgery, sports medicine, wound care, and more. As experts in the lower extremities, podiatrists provide both non-surgical and surgical treatments depending on your diagnosis. Examples include:
Non-Surgical Treatments
- Prescription anti-inflammatory medications, injections, physical therapy, orthotics, immobilization bracing
- Padding and strapping techniques to redistribute pressure
- Nail trimming, debridement of corns/calluses/warts, treatment of athlete’s foot and other fungal infections
- Prescription of therapeutic footwear, custom orthotics, ankle braces, or other supportive devices
- Diabetic foot care like glucose control, wound care, circulation improvement
Surgical treatments
- Bunionectomy (bunion removal) or other soft tissue procedures
- Hammertoe correction
- Removal of bone spurs, ganglion cysts, benign tumors
- Neuroma excision
- Achilles tendon repair
- Ankle arthroscopy, fixation of ligament tears or fractures
- Correction of congenital foot/ankle deformities
- Amputation for severe infections/non-healing wounds in patients with critical limb ischemia
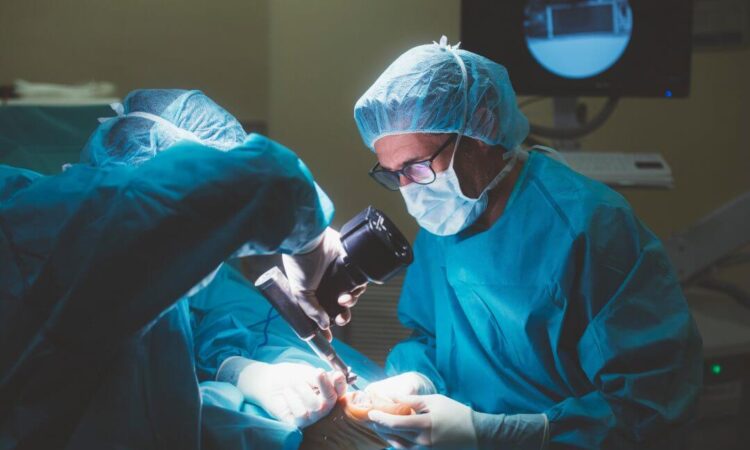
Podiatric surgery is typically performed under local anesthesia or light sedation on an outpatient basis. After surgery, podiatrists provide wound care instructions and recommendations for recovery at home. They also prescribe short-term casting/bracing, crutches, physical therapy, or pain medications to help manage post-op swelling and discomfort. If you want more details, visit here do podiatrists do surgery.
Regular follow-up is important
If foot pain or injury is impacting your daily activities, don’t delay in seeking podiatric care. Podiatrists provide advanced treatments to relieve pain, restore function, get you moving comfortably again, and prevent lasting damage. Ongoing follow-up care is also essential for optimal recovery from foot surgery, wound healing in diabetic patients, custom orthotic prescriptions, and management of chronic conditions like arthritis or tendonitis. Rather than tolerating frustrating foot problems, take charge of your mobility and well-being. Schedule an exam with a podiatrist at the first signs of persistent foot pain, injury, or other concerning lower extremity symptoms. Your feet support your whole body, so be proactive about protecting your long-term health!